“I’m in pain” never means the same thing
Publié il y a 2 mois
19.03.2026
Partager
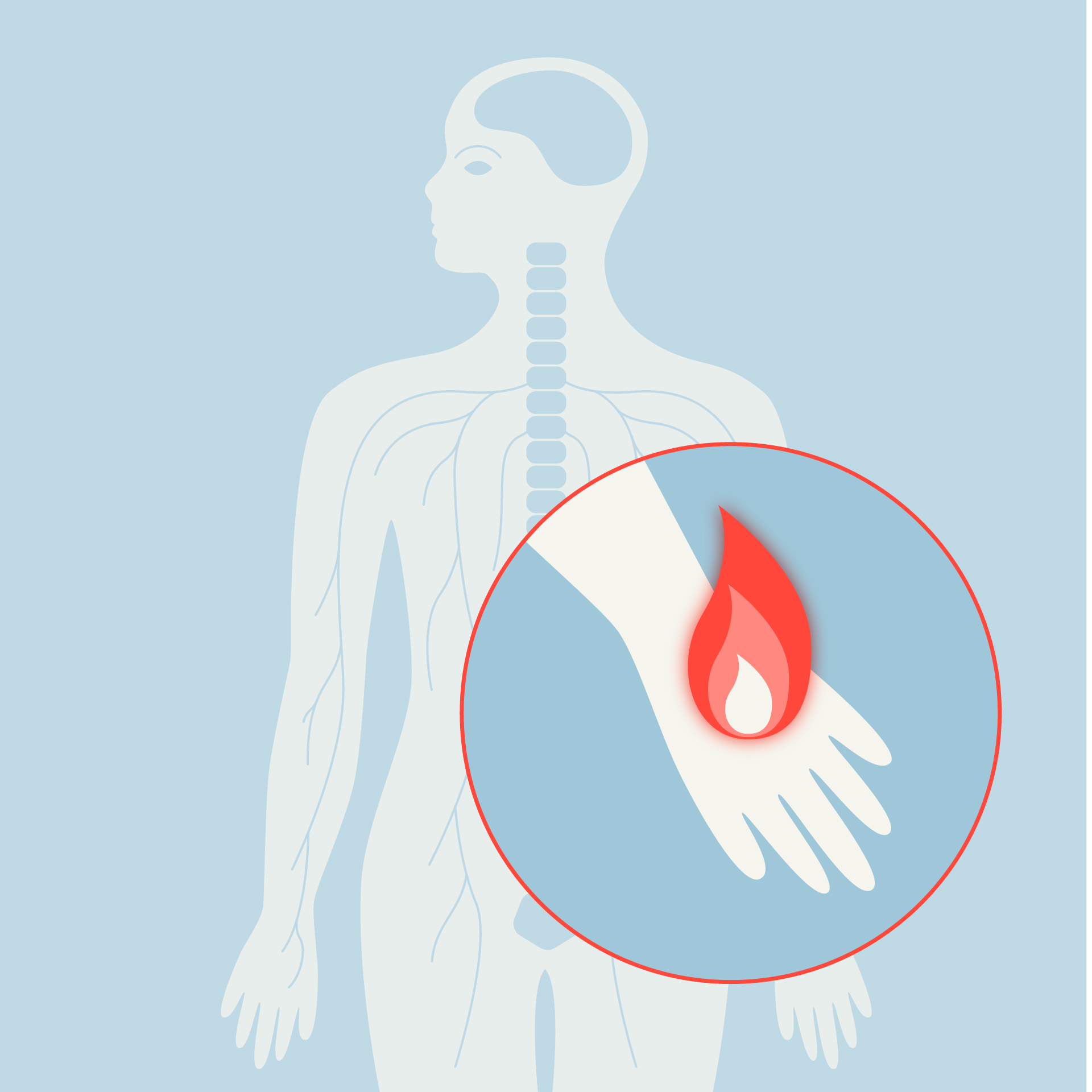
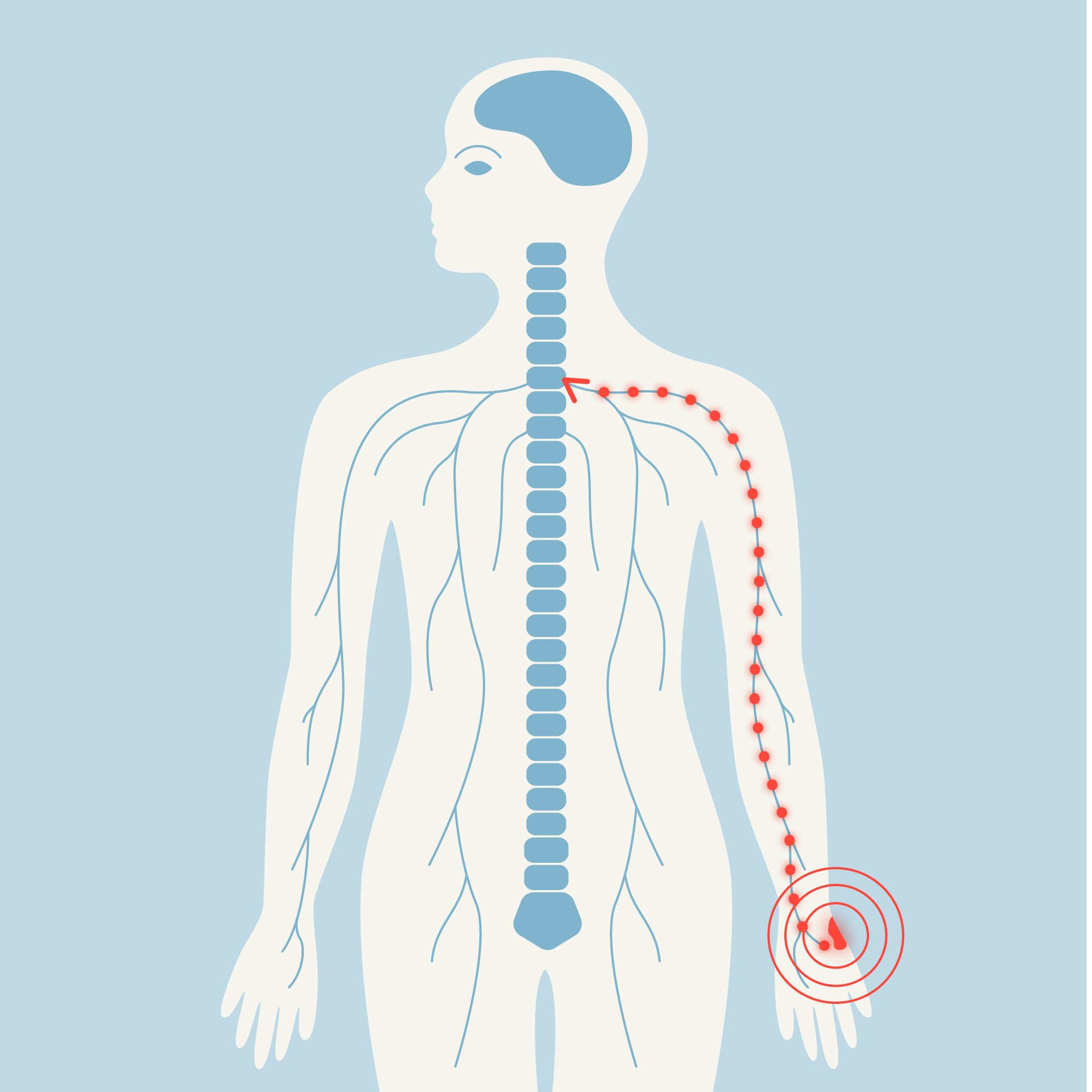
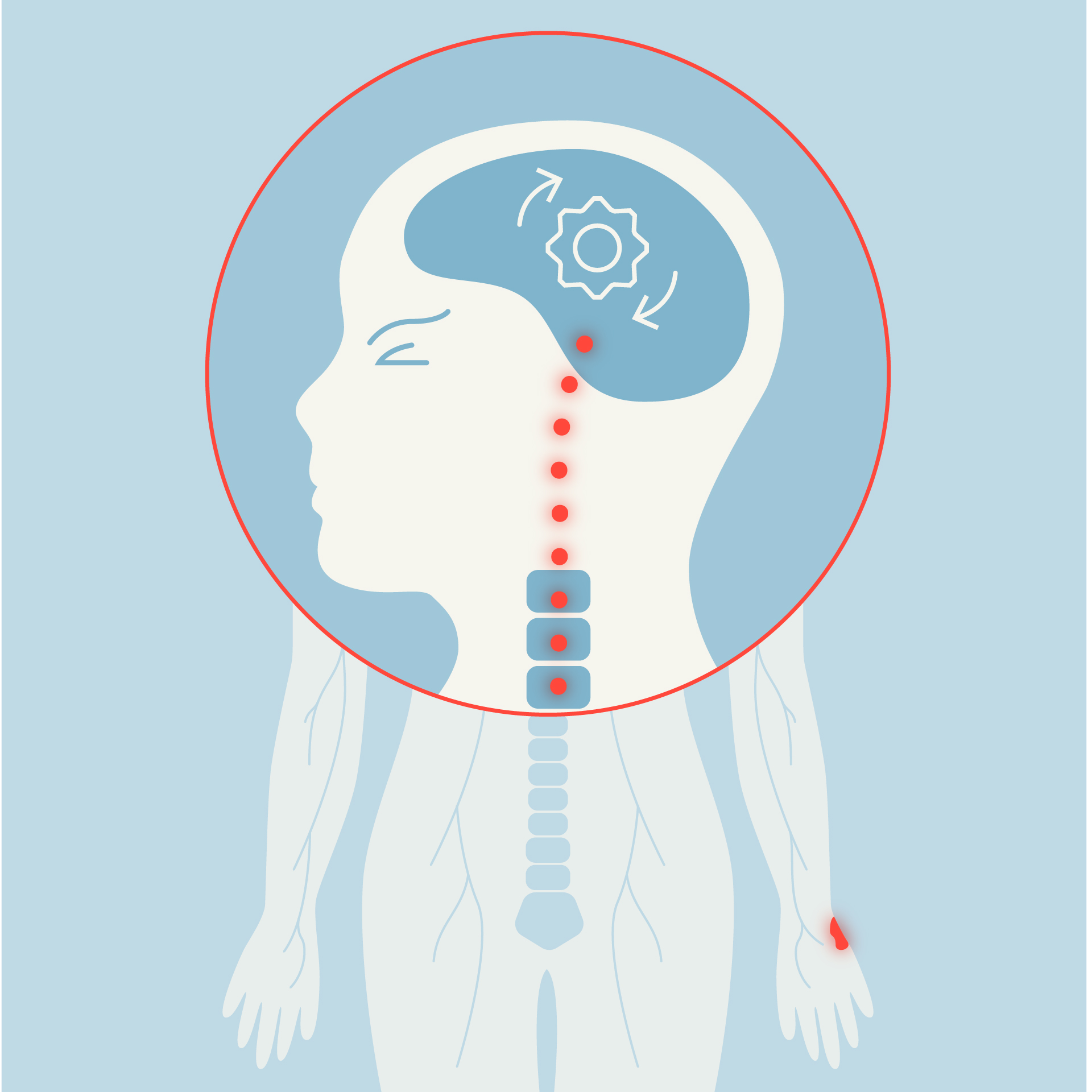
A sharp pain, whether it is a burn, a sting, or intense pressure, originates in the body. Receptors are activated and send an electrical signal along nerves to the spinal cord, where it can be modulated before reaching the brain. When information reaches the brain, it is processed by several distinct brain regions known as the 'pain matrix'. These regions work together to produce the experience of pain, although their exact interactions are still only partly understood.
The brain tells us not only where pain is located, but also how it is experienced. Certain regions enable the precise localisation of pain in the body. Others determine the emotional aspect, shaping whether the pain feels tolerable or overwhelming. “We often describe pain by imagining what being stabbed would be, even if we have never actually been stabbed,” explains Marc Suter, head of the Anaesthesiology Service at CHUV. Conversely, the burning sensation is familiar to almost everyone. Indeed, we often refer to a burning sensation even when there is no actual tissue damage.
It is precisely this paradox that lies at the core of the medical definition of pain: an experience that is both sensory and emotional, unpleasant, and linked to real or potential tissue damage. In other words, pain can occur without visible injury.
Clinicians rely on patients’ descriptions to classify pain according to its mechanisms. Pain caused by nerve damage is not treated the same way as inflammatory joint pain. Treatments vary depending on the suspected origin of the pain.
A personal experience
We are all biologically unique. Nervous system responses, sensitivity thresholds, and the way the brain processes signals vary from person to person. Psychological factors also play a role. Past experiences, traumas, and suffering can amplify pain and make it harder to endure. “A backache may be tolerable under normal circumstances or become unbearable if it occurs after a dismissal, for example.” The social environment also plays a significant role in the experience of pain. Support—or the lack of it—also shapes how pain is perceived.
It is the combination of biological, psychological, and social factors that comprises the biopsychosocial model of pain as described by clinicians. A holistic approach, which is now essential for understanding why the same injury can be experienced so differently by different individuals.
How pain travels through the body
Chronic pain: going beyond the 1 to 10 scale
Within a hospital setting, pain is often assessed using a scale. Patients are asked to rate the severity of their pain, with 1 representing the lowest and 10 the highest. This method is very effective for acute pain, especially in hospital or postoperative contexts. In such cases, the patient's score often corresponds with observable signs, such as grimacing, tension, or complaints. The score can be recorded at each clinical visit, monitored over time, and reduced after treatment. It is a reliable system for temporary pain cases that are expected to improve.
On the other hand, once pain becomes persistent, the scale reveals its limitations. “In chronic pain consultations, patients may report a pain level of 10 out of 10 while still smiling.” There is a clear contrast with acute pain, where maximum intensity is almost always accompanied by crying or shouting. “Patients often say that they cannot cry all day.” In this context, the pain scale tends to lose much of its significance. Moving from 6 to 2 on the scale can then indicate genuine improvement. However, for someone who suffers in multiple areas, who has been at 8 out of 10 for months or even years, lowering this score is no longer the primary goal.
The real question is: what is the impact of pain on daily life? Chronic pain is now recognised as a genuine illness, not just a symptom. The aim is not to ensure a quick recovery but to help the individual live better with the pain, sometimes over the long term.
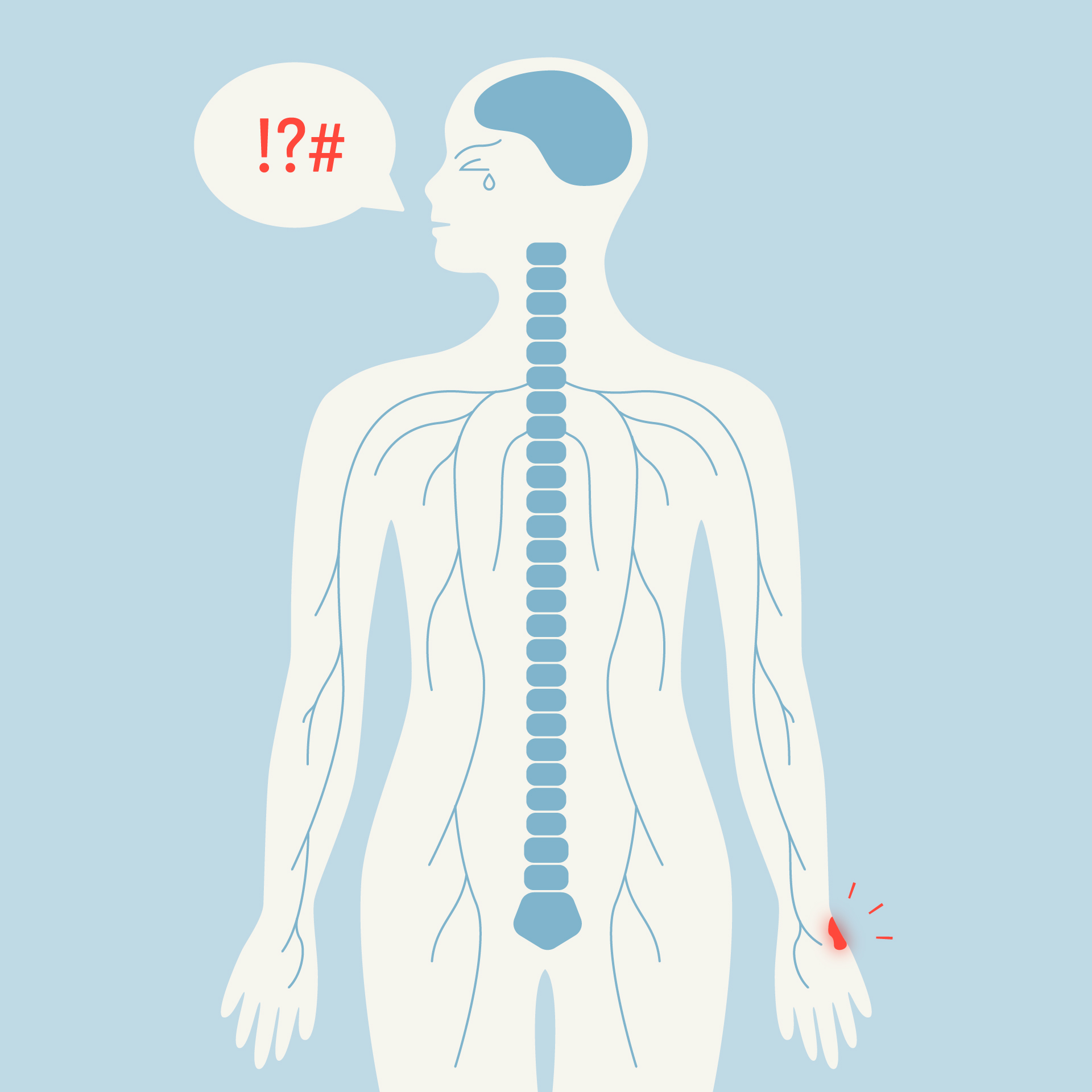
Expressing pain differently
“Some patients have great difficulty accurately describing their pain,” explains Marc Suter. At the Analgesia Centre, we collaborate with psychologists and a psychiatrist to support these individuals, especially those called “alexithymic”—that is, unable to put words to their emotions or feelings.

“Some patients have great difficulty accurately describing their pain,” explains Marc Suter from the CHUV Pain Management Center, department of Anaesthesiology.
With these individuals, speech alone quickly reaches its limits. To overcome this barrier, alternative methods are used, such as music, emotionally evocative cards, art therapy, or painting. These techniques allow one to go beyond verbal language and explore other forms of communication, helping to express aspects of pain or emotion that could not otherwise be verbalised.
Hypnosis follows the same principle. It does not remove the cause of pain but alters how the brain perceives sensations. With practice, some individuals develop highly effective self-hypnotic skills. In certain medical contexts, these techniques are even used to carry out procedures without relying on heavy medication. They show the brain’s influence on pain and offer people with chronic pain a way to actively manage their condition.
Are women more tolerant of pain than men?
This belief is widespread, but it is more a myth than a scientific fact. "Overall, research suggests that women are more sensitive to pain than men," explains the expert. In other words, they perceive a painful stimulus more quickly or intensely. Conversely, when it comes to tolerance, which is the ability to endure pain over time, experiments suggest that they may have greater endurance.
These results, however, should be interpreted with caution. Most of these studies are about twenty years old. In animals, males and females respond differently to central nervous system inflammation. Some treatments that are effective in males are ineffective in females, and vice versa. Despite this, in human medicine, men and women are still often given the same treatments.
"It is possible that in the future, we will develop gender-specific care," says Marc Suter. In animals, observed differences are purely biological. Applying these findings to humans is more complex, particularly when social and cultural factors come into play. In humans, gender, context, and social interactions significantly influence pain responses. Sensory tests can differ depending on whether the person is assessed by a man or a woman, or if a relative is present. “A man tested in the presence of a friend will tend to be less sensitive than if he is alone.”



![[Translate to Anglais:] iStock](https://www.invivomagazine.ch/fileadmin/_processed_/5/6/csm_Fille_casque_bichro_65500bdac2.jpg)